Iatrogenesis (treatment-caused disease)
Nosocomial infection is a major explanation of "COVID deaths"
When patients who tested positive for COVID ended up dying, it was almost always the case that the cause of death was reported as COVID. But evidence suggests that a large fraction, likely a majority, of all of the COVID deaths were due to something else.
Public Enemy #1 (not COVID?)
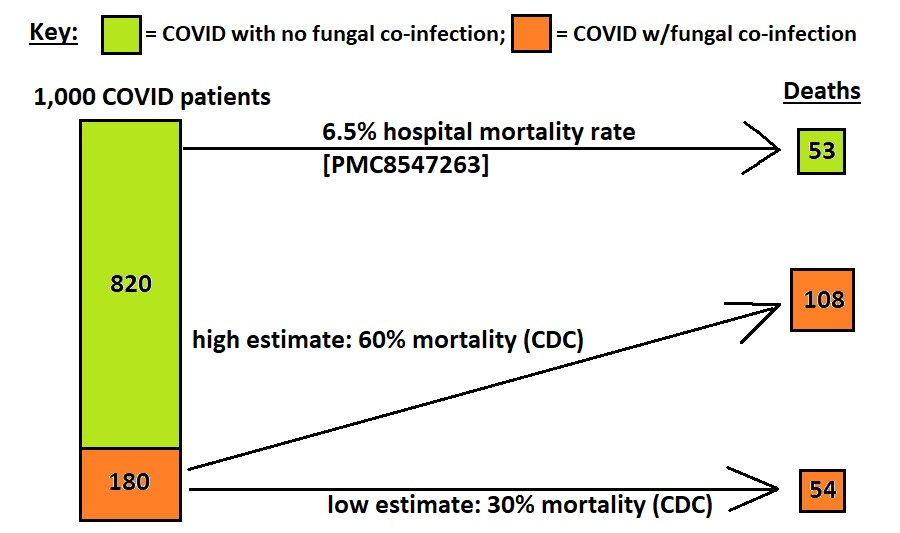
One of the deadliest diseases, often contracted inside of the hospital system, is a drug-resistant, invasive fungal infection. The following graph was made by using a conservative estimate on incidence of fungal co-infection in COVID patients (mixture of severe and non-severe), along with conservative estimates of lethality due to fungal super-infection:
Notice how it is that, even at the low CDC estimate of mortality from a bad fungal co-infection, it is estimated that fungal co-infections killed more of those COVID-hospitalized patients than even COVID did.
An especially bad fungal disease is Candida auris (C. auris) which, unlike other Candida species, can be transferred iatrogenically — i.e., you can get it from receiving care inside of a hospital (a nosocomial infection). It can be deposited on surfaces and remain viable for a long time.
In a recently-published study of those in critical care, 1 in every 3 COVID patients had a fungal co-infection.
In Florida, after noticing C. auris in a few patients in a hospital in July of 2020, CDC and the Florida Dept. of Health monitored the influx of 67 ICU COVID patients in early August and found that 35 (52%) of them tested positive for C. auris.
In Brazil in November 2020, data from two hospitals revealed candidemia (Candida infection of the bloodstream) in hospitalized COVID patients at rates 10-fold higher than typical.
The authors of the study blamed it on the widespread use of corticosteroids for COVID, but the most-used hospital treatment for COVID — i.e., Tocilizumab (a monoclonal antibody) — is also associated with invasive fungal infections.
Other invasive fungal co-infections common with COVID-treated hospital patients are Aspergillus and Mucorales.
Because of under-diagnosis of fungal co-infection — e.g., 60% of invasive pulmonary aspergillosis (IPA) went undiagnosed — it is possible (and even likely) that fungal co-infection is responsible for more than twice the death in hospitalized COVID patients than COVID, itself.
Did we just have a COVID pandemic, or is it more truthful to say that we had a pandemic of iatrogenesis?
Reference
[C. auris on the West Coast; CDC says 30-60% die] — Pierce County man believed to be first in state infected with potentially deadly fungus. https://www.yahoo.com/news/pierce-county-man-believed-first-194944869.html
[193,000 COVID patients with hospital death down to 6.5% by August 2020] — Nguyen NT, Chinn J, Nahmias J, Yuen S, Kirby KA, Hohmann S, Amin A. Outcomes and Mortality Among Adults Hospitalized With COVID-19 at US Medical Centers. JAMA Netw Open. 2021 Mar 1;4(3):e210417. doi: 10.1001/jamanetworkopen.2021.0417. PMID: 33666657; PMCID: PMC8547263. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8547263/
[1 in 3 critical COVID patients had a fungal co-infection] — Negm EM, Mohamed MS, Rabie RA, Fouad WS, Beniamen A, Mosallem A, Tawfik AE, Salama HM. Fungal infection profile in critically ill COVID-19 patients: a prospective study at a large teaching hospital in a middle-income country. BMC Infect Dis. 2023 Apr 18;23(1):246. doi: 10.1186/s12879-023-08226-8. PMID: 37072718; PMCID: PMC10111294. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10111294/
[52% of a sample of COVID patients in Florida had C. auris] — Prestel C, Anderson E, Forsberg K, Lyman M, de Perio MA, Kuhar D, Edwards K, Rivera M, Shugart A, Walters M, Dotson NQ. Candida auris Outbreak in a COVID-19 Specialty Care Unit - Florida, July-August 2020. MMWR Morb Mortal Wkly Rep. 2021 Jan 15;70(2):56-57. doi: 10.15585/mmwr.mm7002e3. PMID: 33444298; PMCID: PMC7808709. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7808709/
[frequency of candidemia in COVID patients in Brazil was 10 times higher than expected] — Riche CVW, Cassol R, Pasqualotto AC. Is the Frequency of Candidemia Increasing in COVID-19 Patients Receiving Corticosteroids? J Fungi (Basel). 2020 Nov 13;6(4):286. doi: 10.3390/jof6040286. PMID: 33203016; PMCID: PMC7712895. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7712895/
[Tocilizumab was “the most used drug in the therapy of COVID-19” but corticosteroids aren’t far behind] — Stasi C, Fallani S, Voller F, Silvestri C. Treatment for COVID-19: An overview. Eur J Pharmacol. 2020 Dec 15;889:173644. doi: 10.1016/j.ejphar.2020.173644. Epub 2020 Oct 11. PMID: 33053381; PMCID: PMC7548059. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7548059/
[60% of invasive pulmonary aspergillosis (IPA) went undiagnosed; and C. auris persists on surfaces] — Hoenigl M, Seidel D, Sprute R, Cunha C, Oliverio M, Goldman GH, Ibrahim AS, Carvalho A. COVID-19-associated fungal infections. Nat Microbiol. 2022 Aug;7(8):1127-1140. doi: 10.1038/s41564-022-01172-2. Epub 2022 Aug 2. PMID: 35918423; PMCID: PMC9362108. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9362108/