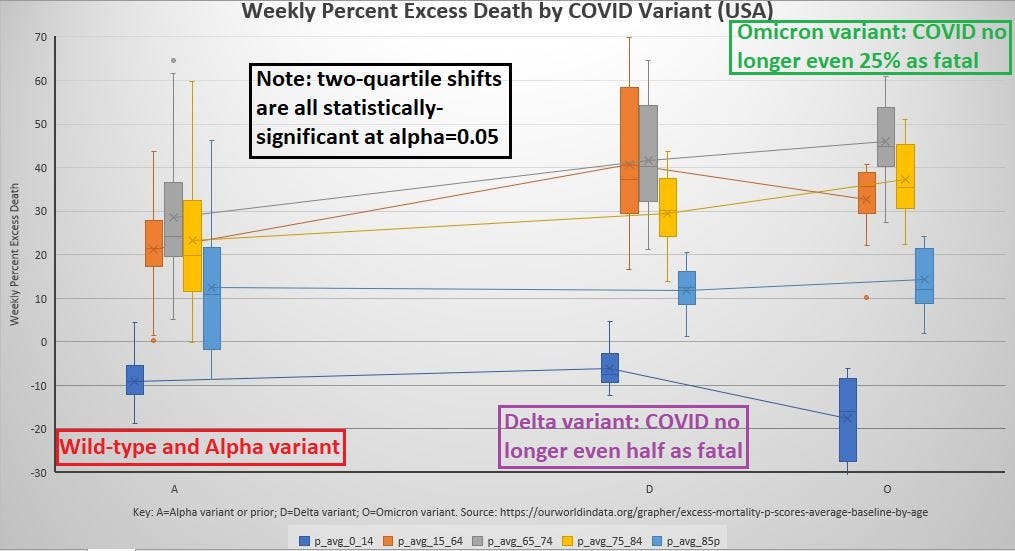
Weekly Excess Mortality vs. COVID Lethality
Evidence of negative correlation: More death as COVID gets weaker
If you look at weekly excess deaths as a percentage above those expected, for the 65 weeks from 29 Mar 2020 to 26 Jun 2021, those deaths correspond to the time when COVID variants were most lethal.
For the 25 weeks from 27 Jun 2021 to 18 Dec 2021, Delta variant predominated, and 700,000 COVID infections followed through time in the UK database reveal that Delta variant was not even half as fatal as Alpha variant was.
For the 10 weeks from 19 Dec 2021 to 20 Feb 2022, Omicron variant predominated, and 1.5 million COVID infections followed through time in the UK database reveal that Omicron is not even half as fatal as Delta (not even a quarter as fatal as wild-type or Alpha).
Yet the median weekly excess deaths rose for some age groups:
The bottom data series represents those under age 15, and excess death data clearly shows that COVID was never a health threat to those under age 15 (all medians are below 0).
If COVID was never a health threat to those under age 15, then COVID vaccines would have a poor risk:benefit ratio in the young (because adverse effects would outweigh health benefits).
In those in the age bracket from 15 to 64 (orange), a two-quartile rise in weekly excess death occurred. I ran a series of R-simulations on quartiles with 250,000 dual samples (data not shown) and discovered that all two-quartile shifts were statistically significant (P < 0.05).
This statistically-significant increase in excess death occurred with the weaker variant, Delta.
Even the age bracket from 65 to 74 (gray) and the one from 75 to 84 (yellow) experienced a statistically-significant quartile-shift (Q2 of Omicron higher than Q3 of Alpha) when comparing Alpha variant to Omicron variant — a variant not even 25% as fatal as Alpha.
How is it that they died less back when the disease was more than 4 times more fatal?
People should not be dying more as COVID gets weaker, and the best explanation for the increase in excess death during COVID variants which are less fatal is that it has to do with the vaccines.
Reference
[OWID data for graph] — Available: https://ourworldindata.org/grapher/excess-mortality-p-scores-average-baseline-by-age
[Table 3: In almost 700,000 cases confirmed by sequencing, Delta was less than half as fatal as Alpha] — UK Technical Briefing #25. Available general: https://www.gov.uk/government/publications/investigation-of-sars-cov-2-variants-technical-briefings
Available specific page: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1025827/Technical_Briefing_25.pdf
[From 1.5 million confirmed cases, Omicron is less than half as lethal as Delta (Omicron is safer than flu)] — Nyberg T, Ferguson NM, Nash SG, Webster HH, Flaxman S, Andrews N, Hinsley W, Bernal JL, Kall M, Bhatt S, Blomquist P, Zaidi A, Volz E, Aziz NA, Harman K, Funk S, Abbott S; COVID-19 Genomics UK (COG-UK) consortium, Hope R, Charlett A, Chand M, Ghani AC, Seaman SR, Dabrera G, De Angelis D, Presanis AM, Thelwall S. Comparative analysis of the risks of hospitalisation and death associated with SARS-CoV-2 omicron (B.1.1.529) and delta (B.1.617.2) variants in England: a cohort study. Lancet. 2022 Mar 16:S0140-6736(22)00462-7. doi: 10.1016/S0140-6736(22)00462-7. Epub ahead of print. PMID: 35305296; PMCID: PMC8926413. Available: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8926413/
[Delta dominant after 26 Jun 2021; Omicron dominant since 19 Dec 2021] — Shi DS, Whitaker M, Marks KJ, et al. Hospitalizations of Children Aged 5–11 Years with Laboratory-Confirmed COVID-19 — COVID-NET, 14 States, March 2020–February 2022. MMWR Morb Mortal Wkly Rep 2022;71:574-581. DOI: http://dx.doi.org/10.15585/mmwr.mm7116e1
[12 total deaths from 37,296 Omicron infections; i.e., 3108 COVID infections required to produce one COVID death (Omicron safer than flu)] — Ulloa AC, Buchan SA, Daneman N, Brown KA. Estimates of SARS-CoV-2 Omicron Variant Severity in Ontario, Canada. JAMA. Published online February 17, 2022. doi:10.1001/jama.2022.2274. Available: https://jamanetwork.com/journals/jama/fullarticle/2789408